Psychiatry:
Towards a Comprehensive
Pathophysiology
of Schizophrenia Based
on Impaired
Glial-Neuronal
Interactions - Part II
By Dr. Bernhard J. Mitterauer
Professor of Forensic Neuropsychiatry
Editor’s Note: Presented
here is Part II of a two-part paper. Part I was featured in the previous
January-February 2013 issue of this Journal.
Pathophysiological model
of schizophrenia
The core symptoms of schizophrenia can be divided into positive and
negative symptoms, with the former including hallucinations, delusions, and
disorganization, and the latter including anergia, flattening of affect, and
poverty of thought content accompanied by significant disturbances in cognitive
function (Meltzer, 2003). Hypotheses concerning the etiology of schizophrenia
comprise biological, psychological and sociological approaches (Carpenter and
Buchanan, 1995; Shastry, 2002; Kapur and Lecrubier, 2003; Lenzenweger et al.,
2007). Generally one can explain delusions and hallucinations in terms of a
“loss of ego- or self-boundaries in the sense of an inner/outer confusion”
(Fisher and Cleveland, 1968; Sims, 1991; Mitterauer, 2003).
Non-functional astrocytic receptors cause astrocytic domain
decomposition
Let me attempt to show how it may be possible to deduce the main
schizophrenic symptoms from an unbalanced tripartite synapse. If the glial
receptors are totally non-functional and therefore cannot be occupied by
neurotransmitters, the system is unbalanced. As in Fig. 6 depicted, the glial
receptors (glR) are non-functional (crosses) and cannot be occupied by
neurotransmitters (NT), so that the activation of the gliotransmitters (GT) is
impossible. Hence, they cannot negatively feedback to the receptors on the
presynapse (prR) and are unable to depolarize the postsynaptic neuron. As a
consequence, the glia lose their inhibitory or boundary-setting function and
the neural transmitter flux is unconstrained, as the flux of thought on the
phenomenological level.
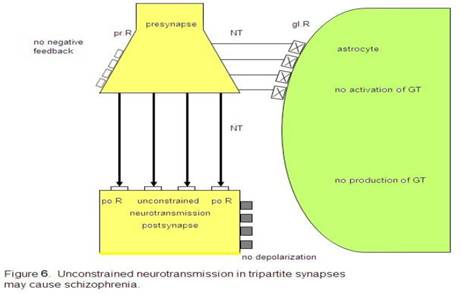
Non-functional
glial receptors (glR), depicted by crosses, cannot be occupied by
neurotransmitters (NT). Since the activation and production of gliotransmitters
(GT) is not possible, glia do not negatively feed back to the presynaptic
receptors (prR) and cannot depolarize the postsynaptic neuron. This severe
synaptic disturbance leads to an unconstrained neurotransmission (fat arrows).
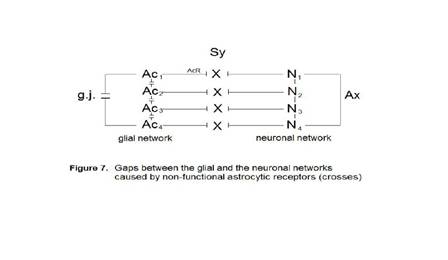
Four
astrocytes (Ac1...Ac4) are interconnected
via gap junctions (g.j.) building a glial network. Four neurons (N1...N4)
are interconnected via axons (Ax) building a neuronal network (dendrites not
shown). The synaptic interactions between the glial and neuronal networks are
interrupted, since the astrocytic receptors (AcR) are nonfunctional (crosses).
As
already described, synaptic glial-neuronal interactions are organized into
astrocyte domains. Non-functional astrocytic receptors decompose the glial
network from the neuronal one causing a gap between the two. Thus, the term
schizophrenia is correct in view of this pathophysiological model. Fig. 7
represents a simple diagram of this network decomposition. Four astrocytes (Ac1…Ac4)
are interconnected by gap junctions (g.j.) building a glial network
(syncytium). Four neurons (N1…N4) are also interconnected
via axons (Ax) generating a neuronal network. Since the astrocytic
receptors (AcR) are non-functional, synaptic glial-neuronal
interactions are disrupted (crosses).
Because
the astrocyte domain organization may be significant for qualitative
information structuring in the brain (Mitterauer, 2010), its decomposition
leads to a generalization of information processing in the neuronal networks.
Thus, schizophrenics cannot recognize qualitatively different features of
subjects and objects but instead they must think in general cases. This
cognitive incapability may cause a misinterpretation of a given reality in the
sense of delusions and hallucinations. One may argue that a glial determination of neuronal networks into functional units is not
necessary because the neuronal system is compartmentalized per se
(Rall, 1995). However, according to my view, there is a qualitative difference
between the purely neuronal compartments and the glia-determined domains.
Neuronal compartments may be merely functional for information processing,
whereas glial-neuronal compartments may in addition have an
information-structuring potency that we need for recognizing the qualitative
differences between objects and individuals in our environment. That capacity
may be lost in schizophrenic patients. Therefore, one can also speak of a loss
of conceptual boundaries in schizophrenia. Let me now deduce the main symptoms
of schizophrenia from unbalanced tripartite synapses caused by non-functional
glial receptors. Table 1 shows the basic schizophrenic symptoms (American
Psychiatric Association, 1998) that may be caused by a loss of conceptual
boundaries. This disorder can affect cognitive processes such as thinking. If a
schizophrenic patient is unable to delimit conceptual boundaries among words,
thoughts, or ideas with different meanings, then meaningless word constructs
(neologisms) or disorganized speech are the typical phenomenological
manifestations, called “thought disorder”.
Table 1.
Interpretation of basic
schizophrenic symptoms
|
Loss of boundaries |
Symptoms |
|
Conceptual |
Thought disorder |
|
Ontological |
Delusions |
|
Perceptive |
Hallucinations |
|
Motoric |
Catatonic symptoms |
|
Emotional |
Affective flattening |
If the loss of boundaries concerns concepts, a thought disorder results.
In the case of a loss of ontological boundaries among the Self and the others
(Non-Selves), delusions occur. This loss of ontological boundaries can also
affect the perception system in the sense of hallucinations. The loss of
boundaries among motor modules shows up in catatonic phenomena. If the
boundaries between emotional qualities are lost, affective flattening is the
typical symptom. (Mitterauer, 2003)
From an ontological point of view, delusions are the consequence of the
loss of boundaries between the self and the others (nonselves). Here, the self
is defined as a living system capable of self-observation (Mitterauer and
Pritz, 1978). One could also say that our brain embodies a distinct ontological
locus of self-observation. Everything taking place in the brains of
schizophrenic patients is reality because they cannot differentiate between
their inner world and the outer world. Therefore, they cannot see ontological
differences between the selves and the nonselves. This loss of ontological
boundaries may lead to a delusional misinterpretation of reality.
Hallucinations may be caused by the same disorder. However, the
perception systems are phenomenologically affected. A schizophrenic who hears
the voice of a person in his head is absolutely convinced that this person is
really speaking to him. The loss of ontological boundaries or inner/outer
confusion shows its phenomenological manifestation in the auditory system. Such
a disorder can also occur in other sensory systems.
If the loss of boundaries affects the motor system in the brain, the
symptomatology is called catatonia. A state of catatonic agitation in which a
disinhibited discharge of nearly all motor systems occurs is an expression of
motor generalization with raging and screaming as behavioral components. One
could also say that the brain’s inability to constrain information processing
among motor modules appears in catatonic phenomena. Hence, the catatonic type
of schizophrenia represents a serious disorder of motor behavior. Typical
symptoms are excessive motor activity and motoric immobility (stupor). Both
phenomena appear to be purposeless and not influenced by external stimuli. In
such a catatonic state, a patient is unable to communicate. He or she cannot
see the other. Everything that happens takes place in the brain of the patient.
Affective flattening is regarded as a negative schizophrenic symptom
(Arajärvi et al., 2006). This symptom can also be explained as a loss of
boundary setting. The different affective or emotional qualities cannot be
produced within the brain, and the communication of feelings is disturbed as a
result (Holden, 2003).
Some genetic considerations
There is growing evidence of disease-related altered astrocyte gene
expression. These findings suggest an imbalance of glutamate-glutamine cycle in
the communication of neurons and astrocytes (Hashimoto et al., 2005). There is
also evidence for a broad involvement of astrocytes in other aspects of the
pathophysiology in schizophrenia (Bernstein et al., 2009). However, if we focus
on nonfunctional receptor proteins on astrocytes, an aberrant splicing may represent
a genetic candidate mechanism. Aberrant or non-splicing causes truncated or
chimeric proteins such that receptor occupancy is not possible. What the
mechanisms of aberrant splicing concerns, significant findings have been
reported (Faa et al., 2010). Nonsense, missense, and even synonymous mutations
can induce aberrant skipping of the mutant exon, producing nonfunctional
proteins. If the exchange of nucleotides generates a synonymous codon that
represents the same aminoacid as the original triplet, one speaks of a silent
mutation. These mutations have erroneously been classified as nonpathogenic,
but are now recognized as affecting the splicing machinery resulting in
defective proteins. Aberrant splicing may play a decisive role in the
pathophysiology of various diseases (Wang and Cooper, 2007). Why not in
schizophrenia, as I hypothesized nearly a decade ago?
Recently, gene losses in the human genome have been identified
(Quintana-Murci, 2012). These loss-of-function variants are located in human
protein-coding genes. Since the first comprehensive, genome-wide catalogue of
variants likely to disrupt protein-coding genes is now available; this genetic
approach could also be promising for the identification of nonfunctional
receptors on astrocytes in brains with schizophrenia. Moreover, epigenetic
factors may also play an important role. Epigenetics broadly refers to
heritable changes in phenotype or gene expression caused by mechanisms other
than changes in the underlying primary DNA sequence. Several major types of
epigenetic mechanisms are DNA methylation, genomic imprinting, histone
modifications, and expression control by noncoding RNA. Recent data suggest the
influence of these epigenetic alterations in schizophrenia (Deng et al., 2010).
Unconstrained neurotransmission may cause demyelination
Generally, in pathological conditions neurotransmitters can be released
excessively, damaging the cells they normally act on. Since oligodendrocytes
have receptors for the various transmitters, neurotransmitter excess can cause
demyelination (Káradóttir and Attwell, 2007). Already in 1977 a study was
published documenting severe breakdown of myelin in dogs injected with myelin
(Saakov et al, 1977). In the grey matter of the brain the death of neurons in
pathological conditions is often caused by a rise of extracellular glutamate
concentration activating NMDA receptors and causing an excessive rise of Ca2+.
Glutamate can also damage white matter oligodendrocytes. Concentrations of
glutamate which alone are not toxic sensitize oligodendrocytes to subsequent
complementary attack that inserts membrane attack complexes into the
oligodendrocyte, allowing a toxic Ca2+ influx to occur (Alberdi et
al, 2006).
In line with the presented synaptic model of the pathophysiology of
schizophrenia, an unconstrained flux of neurotransmitters occurs. This may hold
for all the various neurotransmitter types. This unconstrained flux of
neurotransmitters may affect oligodendrocytes either by flooding of their cognate
receptors on oligodendrocytes, exerting a toxic Ca2+ influx, or via
a hyperactivation of axons with an excess of axonic ATP production and a
consequent toxic effect on oligodendrocytes (Mitterauer and Kofler-Westergren,
2011) (Fig. 8). In addition, ATP released from axons cannot activate astrocytic
receptors, since they do not function. Therefore, a stimulation of myelination
by mature oligodendrocytes is not possible. These pathological mechanisms may
cause demyelination, as observed in brains with schizophrenia (Skelly et al,
2008; Takahashi et al, 2010). Note, although decreased expression of
oligodendrocyte-related genes has been identified (Höstad et al, 2009), it
seems implausible that genetics alone could account for demyelination in
schizophrenia (Fields, 2009).
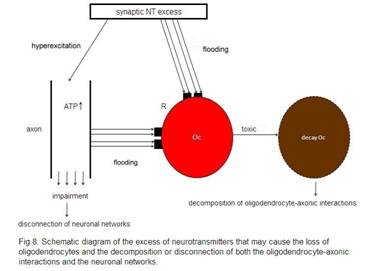
A synaptic
neurotransmitter (NT) excess hyperexcites the axon and floods the cognate
receptors (R) on the oligodendrocyte (Oc). In parallel, a non-synaptic ATP
excess occurs, also flooding R. This flooding of NT and ATP exerts a toxic
effect on the Oc, leading to its decay. These mechanisms may be responsible for
the decomposition of oligodendrocyte-axonic interactions and the disconnection
of neuronal networks.
Moreover, the permanent hyperactivation of axons may also impair them so
that neuronal networks disconnect. This may represent a possible mechanism that
could at least in part be responsible for the disconnection of neuronal
networks identified in brains with schizophrenia (Höstad et al, 2009).
Loss of Oligodendrocytes May Cause a Decay of Gap Junctions in the
Panglial Syncytium Responsible for Memory Impairment
Since gap junctions between astrocytes and oligodendrocytes are
heterotypic, composed of special astrocytic connexins and different
oligodendrocytic connexins, a loss of oligodendrocytes disrupts
astrocyte-oligodendrocytic gap junctions in the panglial syncytium, leading to
a “leaky” syncytium (Fig. 9). Gap junctions form plaques that may embody memory
structures (Robertson, 2002). Therefore, a loss of gap junctions may impair
memory. In addition, genetic or (and) exogenous disorders can affect gap
junctional plaque formation which may be the case in schizophrenia. In this
context one could speak of a syncytiopathy in schizophrenia (Mitterauer, 2009).
However, memory impairment may also be caused by a disorganization of neuronal
networks (Wolf et al, 2008).
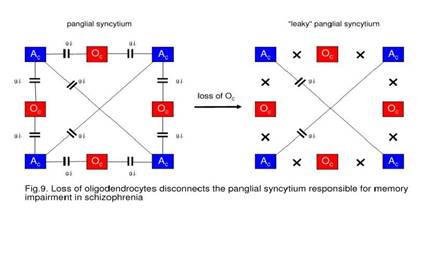
On the left,
a panglial syncytium composed of astrocytes (Ac) and oligodendrocytes (Oc)
interconnected via gap junctions (g.j.). A loss of Oc may cause a decay of
Oc-Ac gap junctions (crosses). Such a “leaky” panglial syncytium may be
responsible for memory impairment.
Schizophrenic dysintentionality based on a severe disorder of
glial-neuronal interactions
According to Frith (1992), schizophrenia can be explained by a failure
to integrate the intention to act with the perceptual registration of the
consequences of that action. At a neurobiological level this integrative
abnormality might correspond to a failure to integrate signals from the
(intentional) prefrontal regions and the (perceptual) temporal cortices.
However, this is a pure neuronal view excluding the glial cell system. In
further elaborating my theory of glial-neuronal interaction, I have
hypothesized that the intentional or action programs of the brain may be
generated in the panglial syncytium (Mitterauer, 2007). Based on a formal model
it can be shown how glial syncytia compute in a highly combinatorial manner
cycles of various lengths via gap junctions. These cycles are transferred in
tripartite synapses to the neuronal system (Mitterauer, 2011). The neuronal
system tests these intentional programs with regard to their feasibility in the
environment. In feeding back the feasibility of intentional programs to the
glial syncytium, learning processes can occur.
For the clinically experienced psychiatrist it is evident that patients
with schizophrenia are unable both to test their delusional programs and to
realize these unrealistic intentions in the environment. I have named this
disorder “schizophrenic dysintentionality” (Mitterauer, 2005). But let us
consider the elementary pathophysiological mechanisms of schizophrenia as
proposed. First of all, there is a break of information processing between the
glial system and the neuronal system in tripartite synapses and also in the
“orthogonal” oligodendrocyte-axonic interaction. In this view, the term
schizophrenia (split of consciousness) is appropriate. In other words: a
patient with schizophrenia is permanently stressed by a world of intentions
that cannot be mediated via tripartite synapses to the neuronal system for
reality testing. Such considerations could be explanatory with concern to
recent findings of abnormalities in the white matter of the brain (Markis et
al., 2010). Supposing that a patient is under permanent pressure to realize
his/her intentional programs generated in the panglial syncytium, then the
normal apoptosis could be accelerated or mutations in astrocytes and in the
oligodendrocyte-myelin system could be activated. The effect is a decrease in
white matter. Considering the loss of oligodendrocytes which are normally
interconnected with astrocytes via gap junctions, the decay of oligodendrocytes
must also destruct the panglial syncytium in the sense of an increasing loss of
gap junctions. This loss of gap junctions may again destruct the capacity of
the panglial syncytium to generate intentional programs.
Many patients with schizophrenia become increasingly psychobiologically
exhausted in the chronic course of their illness, which is called schizophrenic
residuum. Of course, the frequently observed disorders in neuronal networks may
also play a role, but the destruction of the panglial syncytium leading to a
dysintentionality per se, may be basically responsible for the negative view of
life, as typically seen in the schizophrenic residuum. Most impressively, if
the prefrontal cortex is severely affected, these patients are incapable of
planning. Therefore, what they want is merely the satisfaction of simple
biological needs (eating, drinking, smoking, getting money to buy something,
etc.). One could also say that with the destruction of the panglial syncytium
all kinds of destiny are broken down as well.
How could astrocytes react to this disaster? Reactive astrocytosis may
be a compensatory attempt. Reactive astrocytosis occurs prominently in response
to all forms of CNS injury or disease. Recent studies point to the role of
reactive astrocytes in helping to limit tissue degeneration and preserve
function after CNS injury (Sofroniew, 2005). So why not in schizophrenia? If
one interprets the degeneration of the panglial syncytium caused by stress as a
functional brain injury, then reactive astrocytosis may here exert the same
mechanism. However, in schizophrenia astrocytosis may not only react to
injuries of the neuronal system, but also attempt to generate a new astrocytic
syncytium in reaction to the degeneration of the panglial syncytium. In this
way the patient can generate intentional programs and keep a “touch of destiny”
alive. This conjecture is experimentally
testable, if one compares the degree of dysintentionality – defined as the
ability to produce intentions or plans – of schizophrenic patients with and
without reactive astrocytosis.
Finally, reactive astrocytosis can be seen in the light of the
Astrocentric Hypothesis (Robertson, 2002). According to this hypothesis, astrocytes
represent the core cells in the brain that not only control the glial-neuronal
interaction, but also determine the functions within the panglial syncytium.
Therefore, astrocytes may be capable – at least – to attempt repairing
dysfunctions in the panglial syncytium, as may be the case in schizophrenia.
Admittedly, the pertinent findings in brains with schizophrenia are
contradictory. However, astrocytosis (astrogliosis) may not occur widespread in
the brain (Bernstein et al., 2008), but it could represent a local phenomenon.
Pathophysiology of non-schizophrenic delusions
The pathophysiological mechanism of non-schizophrenic delusions may
significantly differ from schizophrenic delusions. Let us focus on the
extrasynaptic fluid, especially Ca2+ ions, in information
transmission. Astrocytes sense a decrease of Ca2+ in the
extrasynaptic space via Cx43 hemichannels and produce ATP that activates
inhibitory interneurons, which negatively feed back to the presynapse. I
hypothesize that if Ca2+ is totally exhausted (e.g. by stress), the
negative feedback mechanism cannot be generated. The exhaustion of Ca2+
may be caused by hyperexcitable neurons flooding the synaptic
neurotransmission. Importantly, the astrocytic receptors are normally
expressed, but they cannot cope with the synaptic neurotransmitter flooding
without an extrasynaptically generated negative feedback. Thus, in
non-schizophrenic delusions an unconstrained information flux may also occur,
but astrocytes per se may not be affected. Here, the brain operates in a
holistic and not schizophrenic way. This pathophysiological mechanism could
explain why patients with paranoid psychoses can mostly be successfully treated
with antipsychotic drugs. Their blockade of postsynaptic receptors constrains neurotransmission
such that astrocytes can work normally again. Although the neurons may remain
hyperexcited, the Ca2+ depletion is sufficient to activate the
negative feedback mechanism described. In parallel, the astrocytic receptors
are again able to modulate synaptic information processing, since they can cope
with the amount of neurotransmitters and temporarily turn off synaptic
information processing based on a negative feedback mechanism.
Do glia play a comparable role in dream states and schizophrenic
delusions?
One of my schizophrenic patients spontaneously told me: “schizophrenia
is dreaming, that’s all”. Here, I will shortly attempt a “gliocentric”
explanation that this patient could be right. Despite progress in biological
sleep or dream research, up to now it is based on an exclusively neuronal
approach (Hobson, 2005). However, the current hypotheses on glial-neuronal
interactions (Robertson, 2002; Mitterauer, 2007; Mitterauer and Kopp, 2003)
could be explanatory what the alteration of consciousness in dreams concerns.
Let me focus on strange dream contents and scenarios. Strange dreams are
defined as dream contents that are unfeasible in wake conscious states. These
are often compared to the main schizophrenic symptoms of delusions and hallucinations.
I hypothesize that the same mechanism may be at work in the generation of both
strange dreams and schizophrenic delusions. It is experimentally verified that
in tripartite synapses astrocytes produce transmitters that occupy receptors on
the presynapse temporarily interrupting synaptic information transmission in
the sense of a negative feedback. In other words: astrocytes have a temporal
boundary-setting function (Mitterauer, 1998). The elementary mechanism may
exert an information structuring function determining the compartmental
organization of neuronal networks.
In schizophrenia, this astrocytic information structuring function may
be lost, since astrocytes do not produce transmitters or express non-functional
receptors because of pertinent mutations. The effect is an unconstrained
information flux in synapses leading to compartmentless neuronal networks in
the sense of a generalization of neuronal information processing. I call this
“loss of self-boundaries in schizophrenia” (Mitterauer, 2003).
Therefore, a patient with schizophrenia is incapable of testing the
reality of his (her) delusional ideas. The phenomenological difference is that
the dreaming person upon awakening is fully able to test the reality. In
contrast, the schizophrenic patient is not. Supposing that our intentional
programs are permanently generated in the glial syncytia (Mitterauer, 2007),
then their realization in the neuronal networks via perception and motion is
decisive. In dreams we have the chance to play our intentions in various
scenarios independent of their feasibility, since the perception systems are
turned off.
Now, it is typical for strange dream scenarios that objects or
individuals of the environmental realities confuse and design uncanny figures
and pictures in the sense of a loss of boundaries. The same glial mechanism
could be responsible as in schizophrenic delusions. However, whereas
schizophrenia represents a chronic pathological process (mutations), dream
states occur as a circadian physiological behavior that gives us the chance of
acting out our hidden intentions without the pressure of their feasibility.
Based on these considerations the elementary function of glia in dream states
could be described as follows: astrocytes temporarily (according to the hypothalamic
circadian rhythms) turn off their interactions with the neuronal system in
tripartite synapses. This mechanism is comparable to that proposed for
schizophrenia. In addition, the generation of intentional programs in the glial
syncytia not only continues, but even dominates the consciousness as dreams
states.
Conclusion
My model of impaired glial-neuronal interactions in schizophrenia is
based on the core hypothesis that nonfunctional astrocytic receptors may cause
an unconstrained synaptic information flux such that glia lose their modulatory
function in tripartite synapses. This may lead to a generalization of
information processing in the neuronal networks responsible for delusions and
hallucinations on the behavioral level. In this acute paranoid stage of
schizophrenia, nonfunctional astrocytic receptors or their loss decompose the
astrocyte domain organization with the effect that a gap between the neuronal
and the glial networks arises. If the illness progresses, the permanent
synaptic neurotransmitter flux may additionally impair the
oligodendrocyte-axonic interactions, accompanied by a “creeping” decay of
oligodendroglia, axons, and glial gap junctions responsible for severe
cognitive impairments. Here we may deal with after-effects caused by the basic
fault of information processing in tripartite synapses. Importantly, the same
may hold true what the neuroinflammatory hypothesis (Brown, 2008) concerns. The
activation of microglia observed in brains with schizophrenia could represent a
reaction to the decay of nervous tissue described and not a primary
pathophysiological mechanism of schizophrenia.
Currently, post mortem brains with schizophrenia are investigated with
Storm microscopy, a method that achieves resolution below the optical
diffraction limit (University of Applied Sciences, Linz, Austria). Whereas in
the prefrontal cortex of normal brains big amounts of receptors located on the
processes of astrocytes are found, in brains with schizophrenia astrocytic
receptors cannot be identified in this region. Since these preliminary results
concern only serotonergic receptors in the prefrontal cortex, further
investigations of other receptor types on astrocytes in pertinent brain regions
is necessary. Should it be possible to verify the central role of astrocytic
receptors in the pathophysiology of schizophrenia, then a diagnostic marker
would be available, if an in vivo identification is possible as well.
Acknowledgements
This paper is dedicated to my friend and great neuroscientist Gerhard
Werner (†), University of Austin, Texas. I am also grateful to Birgitta
Kofler-Westergren for preparing the final version of this paper.
References
Alberdi,
E., Sanchez-Gomez, M.V., Torre, I., Domercq, M., Perez-Samatin, A.,
Pérez-Cerdá, F., Matute, C., 2006.
Activation of kainate receptors sensitizes
oligodendrocytes to complement attack.
J Neurosci. 26, 3220-3228.
American
Psychiatric Association, 1998. Diagnostic and statistical manual of
mental disorders. American Psychiatric
Association, Washington.
Arajärvi,
R., Varilo, T., Haukka, J., Suvissari, J., Suokas, J., Juvonen, H., Muhonen,
M.,
Lönnquist, J., 2006. Affective flattening
and alogia associate
with familial form of schizophrenia.
Psychiatry Res. 141, 161-172.
Araque,
A., Parpura, V., Sanzgiri, R.P., Haydon, P.G., 1999. Tripartite synapses:
glia, the unacknowledged partner. Trends Neurosci. 22, 208-215.
Auld, D.S., Robitaille, R., 2003. Glial cells and
neurotransmission: an inclusive
view of synaptic function. Neuron 40,
389-400.
Berge,
S., Koenig, T., 2008. „Cerebral disconnectivity: an early event in
schizophrenia.”
Neuroscientist 14, 19-45.
Bernstein,
H.G., Steiner, J., Bogerts, B., 2009. „Glial cells in
schizophrenia:
pathophysiological significance and
possible consequences for therapy.” Expert Rev.
Neurother. 9, 1059-1071.
Brown,
A.S., 2008. The risk for schizophrenia from childhood and adulthood infections.
Am. J. Psychiatry 165, 7-10.
Carpenter,
W.T., Buchanan, R.W., 1995. Schizophrenia: introduction and overview,
In: Kaplan, H.J., Sadock, B.J. (Eds.),
Comprehensive Textbook of Psychiatry,
Williams and Wilkins, Baltimore, pp.
899-902.
De-Miguel,
F.F., Fuxe, K., 2012. Extrasynaptic neurotransmission as a way of modulating
neuronal functions.
Front. Physiol. doi:10.3389/fphys2012.00016.
Deng,
Z., Sobell, J.L., Knowles, J.A., 2010. Epigenetic alterations in schizophrenia.
Focus 8, 358-365.
Dermietzel,
R., Spray, D.C., 1998. From neuroglue to glia: a prologue. Glia 24, 1-7.
Di,
X., Chan, R.C., Gong, Q., 2009. White matter reduction in patients with
schizophrenia as revealed by voxel-based
morphometry: an activation likelihood
estimation meta-analysis. Prog.
Neuropsychopharmacol. Biol.
Psychiatry 33, 1390-94.
Erdi,
P., Flaugher, B., Jones, T., Ujfalussy, B., Zalanyi, L., Diwadkar, V.A., 2007.
“Computational approach to
schizophrenia. Disconnection syndrome and dynamical
pharmacology.” AIP Conference
Proceedings 1028, 65-87.
Faa,
V., Cobana, A., Incani, F., Constantino, L., Cao. A., Rosatelli, M.C., 2010.
A synchronous mutation in the CFTR gene
causes aberrant splicing in an italian
patient affected by a mild form of
cystic fibrosis. J. Mol. Diagnostics 12, 380-383.
Fields, R.D., 2009. The other brain, Simon and Schuster, New York.
Fields, R.D., 2010. Change in the brain’s white matter. Science 330,
768-769.
Fields,
R.D., Ni, Y., 2010. Nonsynaptic communication through ATP release
from volume-activated anion channels in
axons. Sci. Signal. 3, ra 73.
Fisher,
S., Cleveland, S.E., 1968. Body image and personality. Dover, New York.
Friston,
K.J., 1998. “The disconnection hypothesis. Schiz. Res. 30, 115-125.
Frith,
C.D., 1992. The cognitive neuropsychology of schizophrenia. Psychology
Press, East Sussex, UK.
Halassa,
M.M., Fellin, T., Haydon, P.G., 2009. Tripartite synapses: roles for
astrocytic purins in the control of
synaptic physiology and behavior.
Neuropharm. 57, 343-346.
Halassa,
M.M., Haydon, P.G., 2010. Integrated Brain Circuits: Astrocytic
Networks Modulate Neuronal Activity and Behavior,
Ann. Rev. Physiol.
72, 335-355.
Hashimoto,
K., Engberg, G., Shimizu, E., Nordin, C., Lindstrom, L.H., Iyo, M.,
2005. Elevated glutamine/glutamate
ratio in cerebrospinal fluid of first episode
and drug naive schizophrenic patients.
BMC Psychiatry 5, 6.
Hobson,
J.A., 2005. Sleep is of the brain, by the brain and for the brain. Nature 437,
1254-1256.
Höstad,
M.N, Segal, D., Takahashi, N., et al., 2009. Linking white and grey matter
in schizophrenia: oligodendrocyte and
neuron pathology in the prefrontal
cortex. Front.
Neuroanat. 3:9. doi;10.3389/neuro.05.009.2009.
Ishibashi, T., Dakin, K.A., Stevens, B., Lee, P.R., Kozlov, S.V., Stewart,
C.L.,
Fields,
R.D., 2006. Astrocytes promote myelination in response to
electrical impulses. Neuron 49,
823-832.
Kapur,
S., Lecrubier, Y., 2003. Dopamine in the pathophysiology and treatment
of schizophrenia. Martin Dunitz,
London.
Káradóttir,
R., Attwell, D., 2007. Neurotransmitter receptors
in the life and death
of oligodendrocytes.
Neuroscience 145, 1426-38.
Kettenmann,
H., Ransom, B.R., 2005. Neuroglia. Oxford
University Press, Oxford.
Kettenmann,
H. and Steinhäuser, C. (2005). „Receptors for neurotransmitters and
Hormones”, in: Kettenmann, H., Ransom,
B.R. (Eds.), Neuroglia, Oxford
University Press, Oxford, pp. 131-145.
Kyriakopoulos,
M., Perez-Iglesias, R., Woolley, J.B., Kamaan, R.A., Vyas, N.S.,
Barker, G.J.,
Frangou, S., McGuire, P.K., 2009. Effect of age at onset
of schizophrenia on white matter
abnormalities. Br. J. Psychiatry 195, 346-353.
Lenzenweger,
M.F., McLachlan, G., Rubin, D.B., 2007. Resolving the latent
structure
of schizophrenia endophenotypes using
expectation-maximization-based finite
mixture modeling. J. Abn. Psychology
116, 16-29.
Markis,
N., Seidman, L.J., Ahern, T., Kennedy, D.N., Caviness, V.S., Tsuang, M.T.,
Goldstein, J.M., 2010. White matter
volume abnormalities and association
with symptomatology in schizophrenia.
Psychiatry Res. 183, 21-29.
Meltzer,
H., 2003. „Multiple neurotransmitters involved in antipsychotic drug action”,
In: Kapur, S., Lecrubier, Y. (Eds.),
Dopamine in the pathophysiology and treatment
of schizophrenia, Martin Dunitz, London,
pp. 177-205.
Mitterauer,
B., 1998. An interdisciplinary approach towards a
theory of
consciousness. BioSystems
45, 99-121.
Mitterauer,
B., 2003. The loss of self-boundaries: towards a neuromolecular theory
of schizophrenia.
BioSystems 72, 209-215.
Mitterauer, B., 2005. Nonfunctional glial proteins in
tripartite synapses:
a pathophysiological model of
schizophrenia. Neuroscientist 11,
192-198.
Mitterauer,
B., 2007. Where and how could intentional programs be generated
in
the brain? A hypothetical model based on glial-neuronal
interactions.
BioSystems 88, 101-112.
Mitterauer, B., 2009. Loss of function of glial gap junctions may cause
severe
cognitive impairments in
schizophrenia. Med. Hypotheses 73, 393-397.
Mitterauer,
B., 2010. Significance of the astrocyte domain organization for
qualitative information structuring in
the brain. Adv.
Biosci. Biotechnol. 1, 391-397.
Mitterauer,
B., 2011. Qualitative information processing in tripartite
synapses: a
hypothetical model. Cogn. Comput. DOI 10.1007/s12559-011-9115-2.
Mitterauer,
B., Kofler-Westergren, B., 2011. Possible effects of
synaptic imbalances
on oligodendrocyte-axonic interactions
in schizophrenia: a hypothetical model.
Front. Psychiatry 2,
doi: 10.3389/fpsyt.2011.00015.
Mitterauer,
B., Kopp, C., 2003. The self-composing brain: towards a
glial-neuronal
brain theory. Brain and
Cognition 51, 357-367.
Mitterauer,
B., Pritz, W.F., 1978. The concept of the self: a theory of
self-observation. Int. Rev. Psychoanal.
5, 179-188.
Newman,
E.A., 2005. “Glia and Synaptic Transmission”, in: Kettenmann, H.,
Ransom, B.R. (Eds.),
Neuroglia, Oxford University Press,
Oxford, pp. 355-366.
Oberheim,
N.A., Wang, X., Goldman, S., Nedergaard, M., 2006. Astrocytic
complexity distinguishes the human
brain, Trends Neurosci. 29, 547-553.
Pereira,
A., Furlan, F.A., 2010. Astrocytes and human cognition: modeling
information integration and modulation
of neuronal activity. Prog.
Neurobiol. 92, 405-420.
Quintana-Murci,
L., 2012. Gene losses in the human genome. Science
335, 806-807.
Ransom, B.R., Ye, Z., 2005. Gap junctions and
hemichannels, in: Kettenmann, H.,
Ransom, B.R. (Eds.), Neuroglia, Oxford
University Press, Oxford, pp. 177-189.
Robertson, J.M., 2002.The Astrocentric Hypothesis: proposed role of
astrocytes
in consciousness and
memory formation. J. Phys. (Paris) 96, 251-255.
Rusakov, D.A., 2012. Depletion of extracellular Ca2+ prompts
astroglia to modulate
synaptic network activity.
Sci. Signal. 5, pe 4.
Saakov,
B.A., Khoruzhaya, T.A., Bardakhchyan, E.A., 1977. Ultrastructural
mechanisms of serotonin demyelination.
Bulleten Eksperimental noi Biologii I
Meditsiny 83, 606-610.
Santello, M., Volterra, A., 2010. Astrocytes as aide-mémoires, Nature 463,
169-170.
Shastry,
B.S., 2002. Schizophrenia: a genetic perspective. Int. J. Mol. Med. 9, 207-212.
Sims,
A., 1991. An overview of the psychopathology of perception; first rank symptoms
as a localizing sign in schizophrenia,
Psychopathology 24, 369-374.
Skelly, L.R., Calhoun, V., Meda, S.A., et al., 2008. Diffusion
tensor imaging
in schizophrenia: relationship to
symptoms. Schizophr.
Res. 98, 157-162.
Steffek,
A.E., 2007. „The role of astrocytes in the pathophysiology of
schizophrenia.”
Dissertation, University of Michigan,
159 pages, 3276299.
Stellwagen,
D., Malenka, R.C., 2006. Synaptic scaling mediated by glial
TNF-alpha. Nature 440, 1054-1059.
Stevens,
B., Porta, S., Haak, L.L., Gallo, V., Fields, R.D., 2002. Adenosine, a
neuron-glial transmitter promoting
myelination in the CNS in response to
action potentials. Neuron 36, 855-868.
Stevens, B., Tanner, S., Fields, R.D., 1998. Control of myelination by
specific patterns
of neural impulses. J.
Neurosci.18, 9303-11.
Takahashi,
N., Sakurai, T., Davis, K.L., Buxbaum, J.D., 2010. Linking
oligodendrocyte and myelin dysfunction
to neurocircuitry abnormalities in
schizophrenia. Prog. Neurobiol. 93,
13-24.
Torres,
A., Wang, F., Xu, Q., Fujita, T., Dobrowolski, R., Willecke, K., Takano, T.,
Nedergaard, M., 2012. Extracellular Ca2+
acts as a mediator of
communication from neurons to glia.
Sci. Sign. 208 ra8.
Wang,
G., Cooper, T.A., 2007. Splicing in disease: disruption of the splicing code
and the decoding machinery. Nature Rev. Gen. 8, 749-761.
Wolf, R.C.,
Höse, A., Frasch, K., Walter, H.,Vasic, N., 2008. Volumetric
abnormalities with cognitive deficits
in patients with schizophrenia.
Eur. Psychiatry 23, 541-548.
Dr. Bernhard Josef Mitterauer
graduated with an M.D. from the University of Graz. Eight years later he
received his academic degree in europsychiatry and Psychoanalysis. Between 1976
and 1984 Dr Mitterauer studied Philosophy with Gotthard Günther, the famous
Philosopher of Cybernetics, in Hamburg. He developed close friendship and intensive scientific
collaboration with Günther, whose philosophy has influenced Dr. Mitterauer’s
work up to this day. In 1984 Dr. Mitterauer was appointed a Professor of Neuropsychiatry
at the University of Graz. He has been serving as a Professor and Head of
Forensic Neuropsychiatry at the University of Salzburg since 1989. He has been
married to Gertraud Laimböck since 1970, and they have a daughter and a son.
Concurrently with his practical work as a Neuropsychiatrist, Dr.
Mitterauer has been involved in interdisciplinary research in Biocybernetics
since the beginning of his professional career. In the 1970’s he published
basic research studies on emotion, depression, narcissism and self-observation.
Notably, in 1981 he earned the Eiselberg Award for his already internationally
acknowledged research on suicide. During the 1980’s he published numerous
studies dealing with a new “dialectic” psychopathology. His book Architectonics, Metaphysics of Feasibility deals
with a future-oriented interpretation of technical activities, especially the
development of robots. An important result of Dr. Mitterauer ’s basic research
is the development of a novel model mental disorders, called “Architectonic
Psychopathology”. Recently he has founded the Volitronics-Institute for Basic
Research, Psychopathology and Brain Philosophy. These research programs are
currently published in international journals and presently in 14 book
publications.
Dr. Mitterauer has patented the most important findings of his
biocybernetic brain research. To date a total of 11 international patents have
been granted to him. He has also developed a new brain theory, which not only
considers the neuronal systems but also accounts for the glial systems of the
brain. Based upon this theory, which was detailed in 1998 in Biosystems, Dr. Mitterauer has shown
that enormous consequences arise from our understanding of consciousness,
psychiatric disorders, and finally, even for the development of “brain-similar”
computers or robots. In addition, concerning his research on consciousness, his
study entitled Some Principles for Conscious Robots, published in
the Journal of Intelligent Systems
in 2000, deserves mention. Based upon his new brain theory, Dr. Mitterauer has
also developed a new type of computer hardware called clocked perception
mechanism.
Having realized that molecular Biology is making fascinating
discoveries, Dr. Mitterauer, in also pursuing this avenue, has postulated
molecular biologically-oriented hypotheses concerning the etiology of Sudden
Infant Death Syndrome, and manic-depressive as well as schizophrenic disorders.
He has also founded the Gotthard Günther Archives for the research and
publication of the posthumous works of Günther at the University of Salzburg.
[ BWW Society Home Page ]
© 2013 The Bibliotheque: World Wide Society